Tech Engineers to Develop a New Catheter to Improve Heart Procedures
April 29, 2026
By Tracie Troha
When patients undergo procedures to open blocked heart arteries, precision matters. Even small imperfections in placing a stent can affect blood flow and long-term health. Now, a research team led by F. Levent Degertekin, Regents’ Entrepreneur, George W. Woodruff Chair in Mechanical Systems, and professor in the George W. Woodruff School of Mechanical Engineering, is working to change that with a new kind of catheter designed to give doctors clearer, real-time insight during these life-saving procedures.
Backed by a four-year, $2.2 million National Institutes of Health Research Project (R01) grant, the project aims to develop a microcatheter that combines high-resolution imaging with precise pressure sensing in a single device.
Personal Inspiration and A Long-Term Vision
Degertekin’s motivation for improving these procedures is deeply personal.
“My brother is an interventional cardiologist,” he said. “It turned out that the ultrasound imaging technologies I’ve been working on were especially suited to address the needs of cardiologists like him.”
That connection helped shape more than two decades of research focused on catheter-based imaging technologies for the heart.
Hidden Problems After Successful Procedures
Each year, more than a million patients in the United States undergo procedures to open blocked coronary arteries. While interventions such as angioplasty and stent placement are routine, they are not always perfect.
Research shows that 24% of patients have residual issues, even when imaging suggests success. In some patients, blood flow is not fully restored, which can lead to complications or additional procedures.
“Nearly one in five cases are complex, and the results are not optimal,” Degertekin explained. “The blood flow is not restored as desired, and there are still pressure drops at the lesion sites.”
Part of the problem lies in how procedures are currently evaluated. Physicians primarily rely on X-ray imaging (fluoroscopy), which shows anatomy but not how well blood is flowing. Measuring that requires additional devices, which adds time, cost, and risk.
A Single Device Providing Multiple Insights
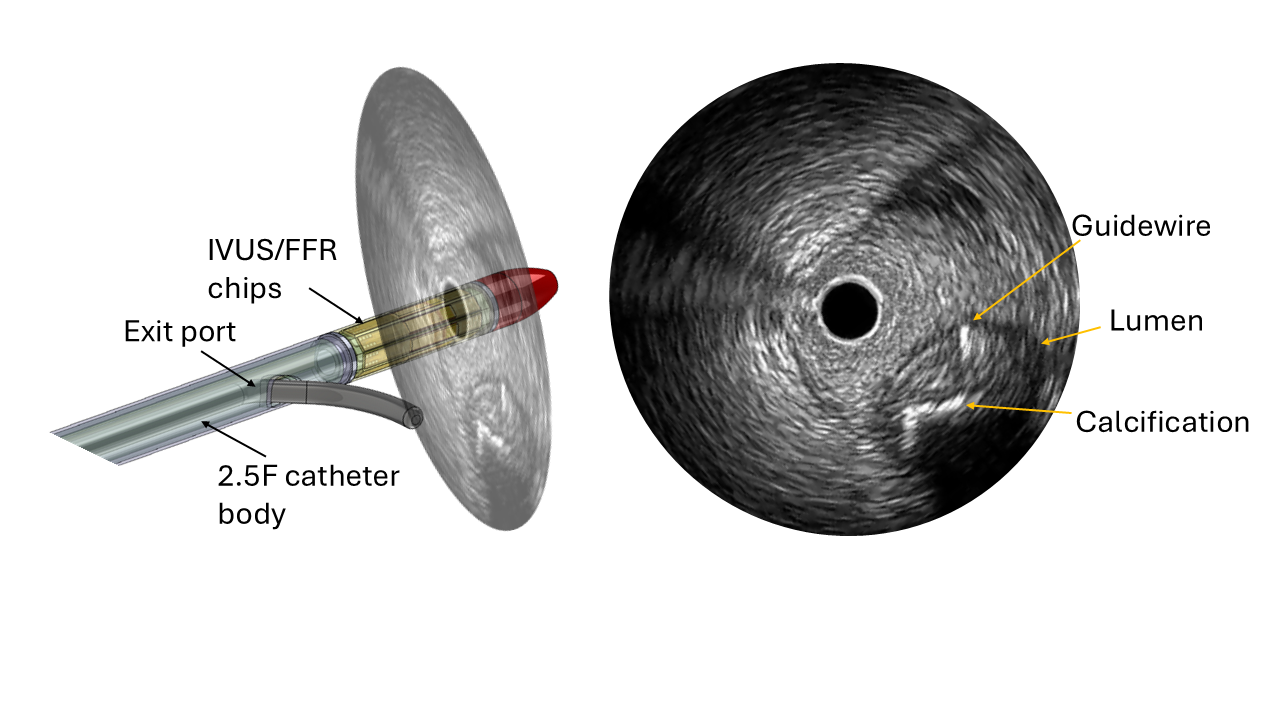
Degertekin’s team is addressing this gap by combining two critical capabilities into one ultra-small catheter: intravascular ultrasound imaging to visualize the artery, and fractional flow reserve sensing to measure blood flow and pressure.
By integrating both functions, the device allows physicians to assess both structure and function at the same time.
“With a single catheter providing both anatomical and physiological information, potential issues can be detected and resolved during the same procedure, reducing the complications,” Degertekin said.
The approach could minimize procedure time and reduce radiation exposure and risk to the patient.
Powered by Silicon Innovation
At the heart of the new device is advanced silicon microelectronics technology.
Using techniques similar to those found in computer chips, the team is integrating ultrasound transducers, pressure sensors, and electronic circuits onto a single silicon platform. This allows the creation of a catheter that is only 800 micrometers in diameter, or less than a millimeter, with nearly 100 tiny transmitters and receivers that are all connected with only eight cables. It’s an engineering feat made possible by combining sensing and electronics on the same chip.
“Only with this small size can one measure pressure accurately in narrow arteries without blocking blood flow,” Degertekin said.
A Collaborative Effort Across Disciplines
The project brings together a multidisciplinary team spanning engineering and medicine, including collaborators from Emory University and Kennesaw State University.
Team members include Yue Chen, associate professor in the Wallace H. Coulter Department of Biomedical Engineering; Shaolan Li, assistant professor in the School of Electrical and Computer Engineering; Coskun Tekes, associate professor of computer engineering at Kennesaw State University (KSU); and Dr. William “Bill” Nicholson, director of interventional cardiology at Emory University.
“This is truly a multidisciplinary project,” Degertekin said. “It requires integrated circuit design, microfabrication, catheter design, and real-time signal processing and beamforming expertise on the engineering side, each of which is a specialization by itself and covered by the Georgia Tech and KSU faculty members.”
Degertekin added that Nicholson’s experience designing and commercializing coronary catheters has been especially valuable in shaping the device for real-world use.
From Lab to Clinic
Over the next four years, the team will design, build, and test the catheter system, moving from benchtop validation to animal studies.
“If we can demonstrate that this technology can perform imaging and pressure sensing as well as the currently separate individual devices in an animal study at the end of the project, that would be a great success,” Degertekin said.
The next steps would include scaling up manufacturing and clinical trials. Encouragingly, some of the underlying fabrication techniques are already used in commercial medical devices, helping lower barriers to translation.
Transforming the Future of Heart Care
Looking ahead, Degertekin believes this technology could have a significant impact, especially in complex cases involving multiple blockages or chronic total occlusions, which can be especially challenging and time-consuming.
“It can potentially improve clinical outcomes, especially for complex interventions,” he said. “The catheter also has special features to help cross chronic total occlusions, which can lead to hours-long procedures.”
By enabling physicians to make better decisions in real time, the technology could lead to safer procedures, fewer complications, and better long-term outcomes for patients.
Eventually, innovations like this could redefine interventional cardiology, making procedures more successful the first time.
